Lots of interesting abstracts and cases were submitted for TCTAP 2023. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge and interact with authors as well as virtual participants by sharing your opinion in the comment section!
TCTAP A-092
Current Risk of Contrast Associated Acute Kidney Injury and Long-Term Outcome After Acute Kidney Injury: Single Centre Experience
By Hafiz Aizat Shuhaimi, Theepa Nesam, Shawal Faizal Mohamad, Noor Diyana Binti Mohamad Farouk
Presenter
Hafiz Aizat Shuhaimi
Authors
Hafiz Aizat Shuhaimi1, Theepa Nesam2, Shawal Faizal Mohamad3, Noor Diyana Binti Mohamad Farouk3
Affiliation
Sultanah Aminah Johor Bahru, Malaysia1, National University of Malaysia, Malaysia2, Hospital Canselor Tuanku Muhriz UKM, Malaysia3
View Study Report
TCTAP A-092
Renal Insufficiency and Contrast Nephropathy
Current Risk of Contrast Associated Acute Kidney Injury and Long-Term Outcome After Acute Kidney Injury: Single Centre Experience
Hafiz Aizat Shuhaimi1, Theepa Nesam2, Shawal Faizal Mohamad3, Noor Diyana Binti Mohamad Farouk3
Sultanah Aminah Johor Bahru, Malaysia1, National University of Malaysia, Malaysia2, Hospital Canselor Tuanku Muhriz UKM, Malaysia3
Background
Contrast associated Acute Kidney Injury (CA-AKI), is one of the known complications and it has been important consideration in patient who undergoing cardiac catheterization. CA-AKI has been associated with kidney failure requiring kidney replacement therapy, mortality, and long-term reduction of kidney function. We evaluated incidence of CA-AKI and kidney outcomes 3 years post coronary angiography.
Methods
Data were collected and analysed for patients who underwent elective coronary catheterization using OMNIPAQUE 350 as contrast agent from 2017 to 2018 with follow up data for 3 years in Hospital Canselor Tuanku Muhriz, Malaysia. Patients who underwent emergency coronary catheterization, end-stage kidney disease patients on kidney replacement therapy, and missing data for analysis were excluded.
Results
179 patients were recruited in this study. The mean age of the study cohort was 61.75 ±10.72 years, 70.4% were men. Baseline kidney function showed mean serum creatinine was 106.4±45.6 µmol/L with eGFR of 71 ±22.8 ml/min/1.73m2 and mean UPCI was 0.1 ±0.18 g/mmol creatinine. Majority were non-smokers (78.2%) and hypertension (80.4%). 60.9% of them were diabetic and mean Hba1c was 7.1 ±1.7 %. 69.8% of them had ACE or ARB as hypertensive medication.
Most of them underwent coronary catheterization due to recent ACS (84.3%), and procedure was COROS without PCI (63.7%) by the radial artery approach (58.1%). Average contrast media given was 122.5 (±68.5) ml,60.3% of the patient received less than 100mls. The mean MEHRAN score calculated was 5 ±3, and 60.3% of our study patients were categorized as low risk of developing CA-AKI.
In our study centre, the incidence of CA-AKI is 3.4%. 38.5% of them had CKD progression by advancing to the next stage of CKD, whilst 2.8% died, while 2.2% became dialysis-dependent at 3 years.
Multiple logistic regression analysis showed nephrotic range proteinuria was significant predictor for CKD progression, death, and dialysis dependant with a p-value of 0.015, 0.037 and 0.003, respectively. Hyponatraemia appears to be a significant predictor for CA-AKI (p 0.042)
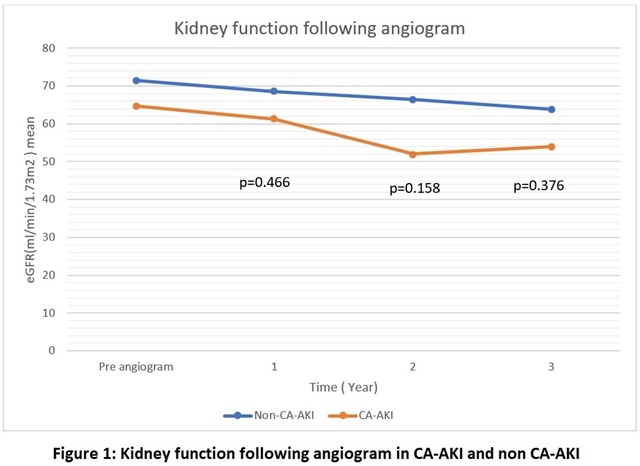
Most of them underwent coronary catheterization due to recent ACS (84.3%), and procedure was COROS without PCI (63.7%) by the radial artery approach (58.1%). Average contrast media given was 122.5 (±68.5) ml,60.3% of the patient received less than 100mls. The mean MEHRAN score calculated was 5 ±3, and 60.3% of our study patients were categorized as low risk of developing CA-AKI.
In our study centre, the incidence of CA-AKI is 3.4%. 38.5% of them had CKD progression by advancing to the next stage of CKD, whilst 2.8% died, while 2.2% became dialysis-dependent at 3 years.
Multiple logistic regression analysis showed nephrotic range proteinuria was significant predictor for CKD progression, death, and dialysis dependant with a p-value of 0.015, 0.037 and 0.003, respectively. Hyponatraemia appears to be a significant predictor for CA-AKI (p 0.042)

Conclusion
The incidence of CA-AKI is relatively low in our study due to low osmolarity and low volume of the contrast. Hyponatraemia appears to be a significant factor associated with development of CA-AKI. CA-AKI patients did not increase the risk of long-term decline in kidney function and survival. Coronary catheterization appears to be safe and low risk developing CA-AKI


