Lots of interesting abstracts and cases were submitted for TCTAP 2023. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge and interact with authors as well as virtual participants by sharing your opinion in the comment section!
TCTAP A-044
Early Mechanical Circulatory Support in Myocardial Infarction Complicated by Cardiogenic Shock: A Nationwide Experience in Comparison to International Experience
By Khaled Al Khodari, Alaa Rahhal, Raad Tahtouh, Mohammed Awad Ashour, Eman Shehada, Wael Kanjo, Mohamad Safwan Aljafar, Mona Sofi, Abdelaziz M Tawengi, Mohamed Mahmoud Tawengi, Abdul Rahman Arabi
Presenter
Khaled Al Khodari
Authors
Khaled Al Khodari1, Alaa Rahhal1, Raad Tahtouh1, Mohammed Awad Ashour1, Eman Shehada1, Wael Kanjo1, Mohamad Safwan Aljafar2, Mona Sofi2, Abdelaziz M Tawengi3, Mohamed Mahmoud Tawengi3, Abdul Rahman Arabi1
Affiliation
Hamad Medical Corporation, Qatar1, Hamad Medical Corporation (HMC), Doha, Qatar2, Qatar University, Qatar3
View Study Report
TCTAP A-044
Hemodynamic Support and Cardiogenic Shock
Early Mechanical Circulatory Support in Myocardial Infarction Complicated by Cardiogenic Shock: A Nationwide Experience in Comparison to International Experience
Khaled Al Khodari1, Alaa Rahhal1, Raad Tahtouh1, Mohammed Awad Ashour1, Eman Shehada1, Wael Kanjo1, Mohamad Safwan Aljafar2, Mona Sofi2, Abdelaziz M Tawengi3, Mohamed Mahmoud Tawengi3, Abdul Rahman Arabi1
Hamad Medical Corporation, Qatar1, Hamad Medical Corporation (HMC), Doha, Qatar2, Qatar University, Qatar3
Background
Timely mechanicalcirculatory support (MCS) to maintain end-organ perfusion is essential inpatients with cardiogenic shock (CS). We report Qatar Cardiogenic ShockExperience (Q-CSE) in providing early MCS among patients with acute myocardialinfarction complicated by cardiogenic shock (AMI-CS) requiring intra-aorticballoon pump (IABP) support in comparison to the National Cardiogenic ShockInitiative (NCSI) in the United States and the Japan registry for Percutaneous VentricularAssist Device (J‑PVAD).
Methods
Q-CSE included all patients admitted with AMI-CS requiring IABP guided by right heart catheterization (RHC) between January 2012 and December 2021 to the national tertiary cardiology center. Survival outcomes including mortality at 30 and 360 days were assessed. Characteristics and outcomes observed in Q-CSE were compared to the latest published results of NCSI and J‑PVAD that used Impella as MCS.
Results
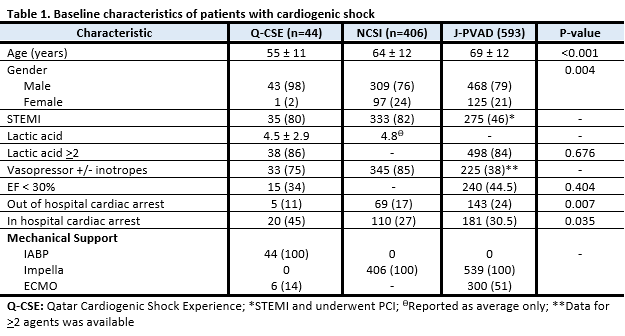
A total of 44 patients were included in the Q-CSE (male: 98%, age: 55 +/- 11 years). In comparison to the NCSI (n= 406) and J‑PVAD (n= 593), our patients were significantly younger, had less out of hospital cardiac arrest, and higher incidence of in-hospital cardiac arrest as demonstrated in Table 1. Among the patients in the Q-CSE, 14% had Extracorporeal Membrane Oxygenation (ECMO) implanted along with IABP, while 51% had ECMO with Impella support in J‑PVAD. Mortality at 30 days was lower in Q-CSE with 19% versus 23% in NCSI, and 37% in J‑PVAD. Similarly, the 360-day mortality was lower in Q-CSE compared to NCSI, 27% versus 38%.

Conclusion
Timely MCS following the NCSI in AMI-CS with IABP to maintain organs perfusion may yield favorable outcomes. A hypothesis-generating observation that may reassure cardiologists to use IABP in a timely manner to achieve favorable outcomes.


