Lots of interesting abstracts and cases were submitted for TCTAP 2022. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge and interact with authors as well as virtual participants by sharing your opinion in the comment section!
TCTAP A-011
The Burden of Short-term Major Adverse Cardiac Events and Its Determinants After Emergency Percutaneous Coronary Revascularization: A Prospective Follow-up Study
By Rajesh Kumar, Nadeem Qamar, Tahir Saghir, Jawaid Akbar Sial, Naveedullah Khan, Musa Karim
Presenter
Rajesh Kumar
Authors
Rajesh Kumar1, Nadeem Qamar1, Tahir Saghir1, Jawaid Akbar Sial1, Naveedullah Khan1, Musa Karim1
Affiliation
National Institute of Cardiovascular Diseases, Pakistan1
View Study Report
TCTAP A-011
Acute Coronary Syndromes (STEMI, NSTE-ACS)
The Burden of Short-term Major Adverse Cardiac Events and Its Determinants After Emergency Percutaneous Coronary Revascularization: A Prospective Follow-up Study
Rajesh Kumar1, Nadeem Qamar1, Tahir Saghir1, Jawaid Akbar Sial1, Naveedullah Khan1, Musa Karim1
National Institute of Cardiovascular Diseases, Pakistan1
Background
Primarypercutaneous coronary intervention (PCI) remains recommended reperfusiontherapy for patients with acute ST-elevation myocardial infarction. This studyaimed to evaluate the short-term major adverse cardiac events (MACE) and theirdeterminants among patients who underwent primary PCI at a tertiary carecardiac center of Karachi, Pakistan.
Methods
Acohort of patients who underwent primary PCI were followed for the MACE.Multivariable Cox-regression analysis was performed with backward conditionalvariable selection and hazard ratio (HR) along with 95% confidence interval(CI) were obtained.
Results
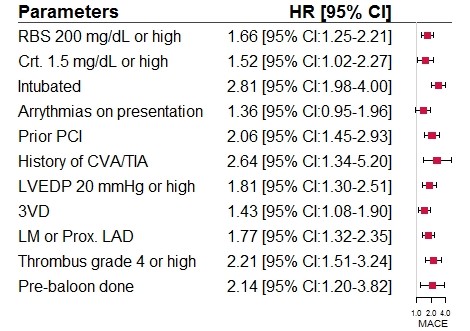
Atotal of 1150 patients were included, of which follow-up was successful in95.8% (1102) and mean follow-up duration was 5.97±2.32 months. MACE wereobserved in 201 (19.1%) patients with 14.2% (157) all-cause mortality, 5.4% (60)cardiac mortality, 0.7% (8) stroke, 3.6% (40) re-hospitalization due to heartfailure, and 6.1% (67) myocardial infarction requiring revascularization.Independent predictors of short-term MACE were found to be admission glucose≥200 mg/dl (1.66 [1.25-2.21]), serum creatinine ≥1.5 mg/dl (1.52 [1.02-2.27]), intubation (2.81[1.98-4.00]), history of PCI (2.06 [1.45-2.93]), history of cerebrovascular accident (2.64 [1.34-5.2]), left ventricular end-diastolic pressure ≥20 mmHg (1.81 [1.3-2.51]), triple vessel diseases (1.43 [1.08-1.9]), culprit left main or proximal left anterior descending artery (1.77 [1.32-2.35]), pre-ballooning (2.14[1.2-3.82]), and thrombus grade≥4 (2.21 [1.51-3.24]).

Conclusion
Asignificant number of individuals undergone primary PCI are still vulnerable tosubsequent short-term MACE, hence, systematic follow-up and early riskstratification should be considered as an integral part of STEMI managementprotocol specially for patients with high-risk features as highlighted herein.


