Lots of interesting abstracts and cases were submitted for TCTAP 2022. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge and interact with authors as well as virtual participants by sharing your opinion in the comment section!
TCTAP A-027
Impact of Left Ventricular Ejection Fraction (EF) on 10-year Mortality After PCI or CABG in the SYNTAXES Trial: CABG Safer than PCI in Reduced Ejection Fraction (rEF)
By Shinichiro Masuda, Kai Ninomiya, Shigetaka Kageyama, Michael J. Mack, A. Pieter Kappetein, Marie-Claude Morice, Yoshinobu Onuma, Patrick W. Serruys
Presenter
Shinichiro Masuda
Authors
Shinichiro Masuda1, Kai Ninomiya2, Shigetaka Kageyama1, Michael J. Mack3, A. Pieter Kappetein4, Marie-Claude Morice5, Yoshinobu Onuma1, Patrick W. Serruys1
Affiliation
University of Galway, Ireland1, Iwate Medical University, Japan2, Baylor University Medical Center, USA3, Erasmus University Rotterdam, Netherlands4, CERC, France5
View Study Report
TCTAP A-027
Bifurcation/Left Main Diseases and Intervention
Impact of Left Ventricular Ejection Fraction (EF) on 10-year Mortality After PCI or CABG in the SYNTAXES Trial: CABG Safer than PCI in Reduced Ejection Fraction (rEF)
Shinichiro Masuda1, Kai Ninomiya2, Shigetaka Kageyama1, Michael J. Mack3, A. Pieter Kappetein4, Marie-Claude Morice5, Yoshinobu Onuma1, Patrick W. Serruys1
University of Galway, Ireland1, Iwate Medical University, Japan2, Baylor University Medical Center, USA3, Erasmus University Rotterdam, Netherlands4, CERC, France5
Background
Coronary artery bypass grafting (CABG) has been recommended in European Society of Cardiology (ESC) guidelines as a standard treatment for patients with multivessel coronary artery disease (CAD) and severely impaired left ventricular ejection fraction (LVEF); however, the impact on vital prognosis at very long-term of percutaneous coronary intervention (PCI) and CABG in patients with reduced ejection fraction remains to be elucidated.
Methods
The present report is a predefined subgroup analysis of the SYNTAXES study (NCT03417050). A total of 1,800 randomized patients with stable de novo three vessel disease and/or left main CAD were categorized into three groups according to the current guidelines of the ESC (1) reduced ejection fraction (rEF; LVEF≤40%), (2) mildly reduced ejection fraction (mrEF; LVEF 41-49%), (3) preserved ejection fraction (pEF; LVEF≥50%). The primary endpoint was 10-year all-cause mortality.
Results
The entire randomized population was stratified as rEF (n = 168), mrEF (n = 179), and pEF (n = 1453). The rates of 10-year all-cause death were 44.0% vs. 31.8% vs. 22.6% (P < 0.001), according to LVEF subgroups (rEF, mrEF and pEF). Among the patients with rEF, there was a tendency toward higher 10-year mortality in PCI group, but the difference was not significant (52.9% after PCI vs 39.6% after CABG, P = 0.054). There were no significant differences in the sub-group of with mrEF (36.0% after PCI vs. 28.6% after CABG, P = 0.273), and pEF, (23.9% after PCI vs. 22.2% after CABG, P = 0.275) respectively. Regarding the 10-year all-cause mortality, there was a significant interaction between LVEF subgroups at 5-year follow-up (P value for interaction 0.049); however, the difference disappeared at 10-year follow-up (P value for interaction 0.183).
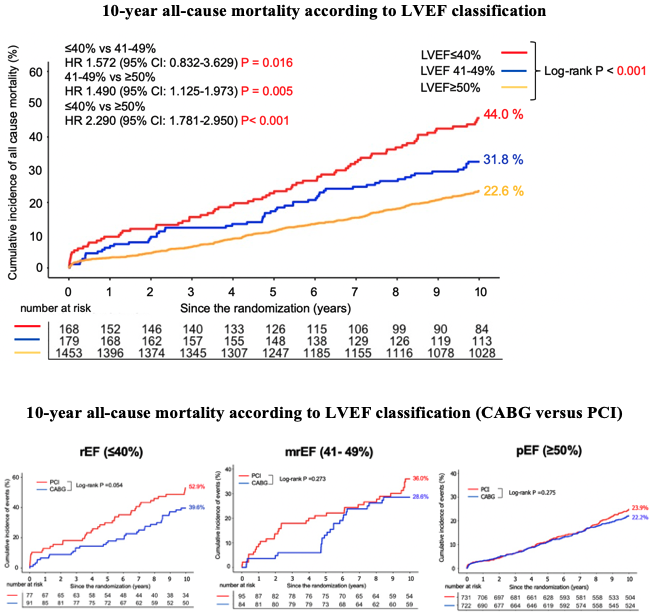

Conclusion
Considering a significantly reduced mortality at 5 years and a numerical trend towards lower 10-year mortality in CABG than PCI among patients with reduced EF, CABG might be a safer revascularization strategy than PCI for patients with EF of less than 40%.


