Lots of interesting abstracts and cases were submitted for TCTAP 2022. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge and interact with authors as well as virtual participants by sharing your opinion in the comment section!
TCTAP A-025
"Do Women Truly Have Worst Outcomes?" Comparison of Outcome Differences for Percutaneous Coronary Intervention in Unprotected Left Main Disease -A Propensity Matched Analysis
By Mugilan Sundarajoo, Quah Wy Jin, Kumara Gurupparan Ganesan, Jayakhanthan Kolanthaivelu, David Yong, Kogulakrishnan Kaniappan, Low Ming Yoong
Presenter
Mugilan Sundarajoo
Authors
Mugilan Sundarajoo1, Quah Wy Jin2, Kumara Gurupparan Ganesan2, Jayakhanthan Kolanthaivelu3, David Yong2, Kogulakrishnan Kaniappan2, Low Ming Yoong2
Affiliation
National Heart Institute Ijn, Malaysia1, National Heart Institute, Malaysia2, Cardiovascular Sentral Kuala Lumpur, Malaysia3
View Study Report
TCTAP A-025
Bifurcation/Left Main Diseases and Intervention
"Do Women Truly Have Worst Outcomes?" Comparison of Outcome Differences for Percutaneous Coronary Intervention in Unprotected Left Main Disease -A Propensity Matched Analysis
Mugilan Sundarajoo1, Quah Wy Jin2, Kumara Gurupparan Ganesan2, Jayakhanthan Kolanthaivelu3, David Yong2, Kogulakrishnan Kaniappan2, Low Ming Yoong2
National Heart Institute Ijn, Malaysia1, National Heart Institute, Malaysia2, Cardiovascular Sentral Kuala Lumpur, Malaysia3
Background
Significant left main stem disease is observed with increasing incidence, given the progressively older patients with higher prevalence of cardiovascular risk factors . Left main stem disease has a significant impact on the symptomatic and prognostic outcome, with a controversial debate regarding the optimal treatment. Many studies have been performed to investigate the gender difference in in-hospital outcomes in patients undergoing PCI, but their results are still conflicting. Most studies reporting the gender issue were conducted in Western countries and Asian data is scarce.Our study aims to examine the impact of gender in patients treated by PCI to unprotected left main stem disease so that we will be able to better risk stratify and plan further management for this group of patients.

Methods
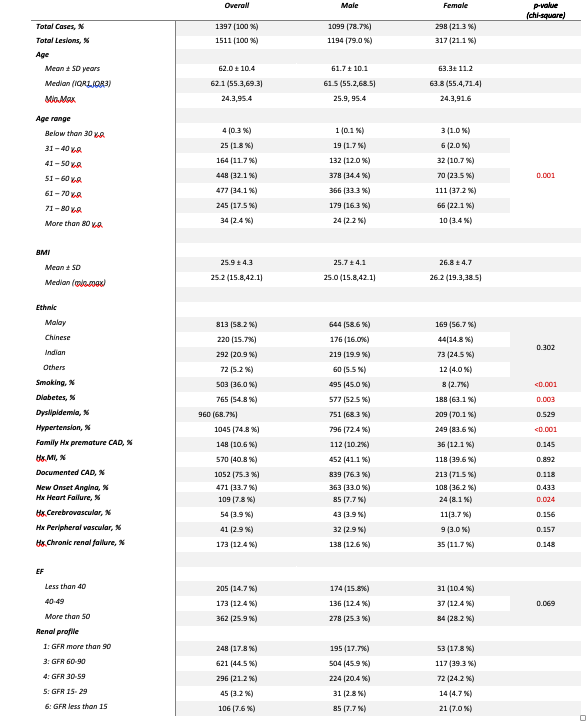
This is a retrospective cohort study done involving a multi-ethnic community in the National Heart Institute, Malaysia looking into the impact of gender in patients treated for Left Main Stem (LMS) disease. The study enrolled 1511 patients undergoing PCI to unprotected LMS from 2007 to 2017. Propensity score matching was performed to adjust for differences in baseline clinical characteristics, yielding a total of 596 patients. Primary outcome is Net Adverse Clinical Event which includes Major Adverse Cardiac and Cerebrovascular Event (MACCE)- all cause death, myocardial infarction, target lesion revascularization, stroke and bleeding.


Results
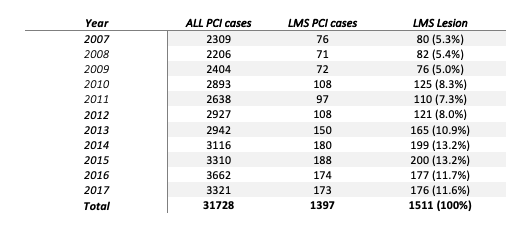
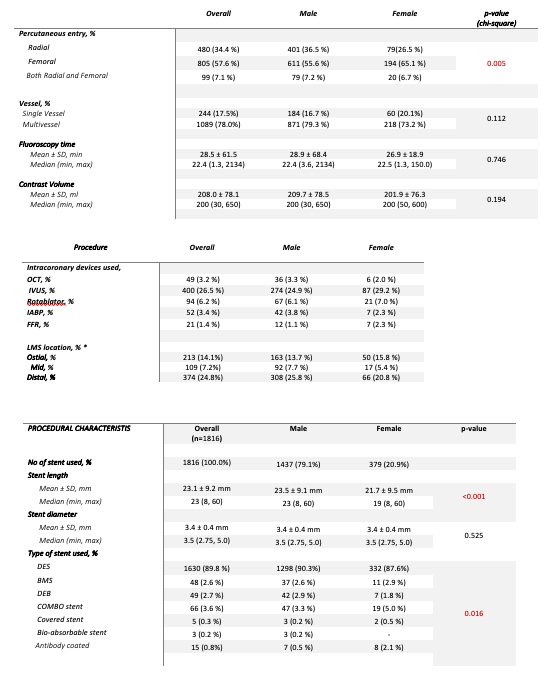
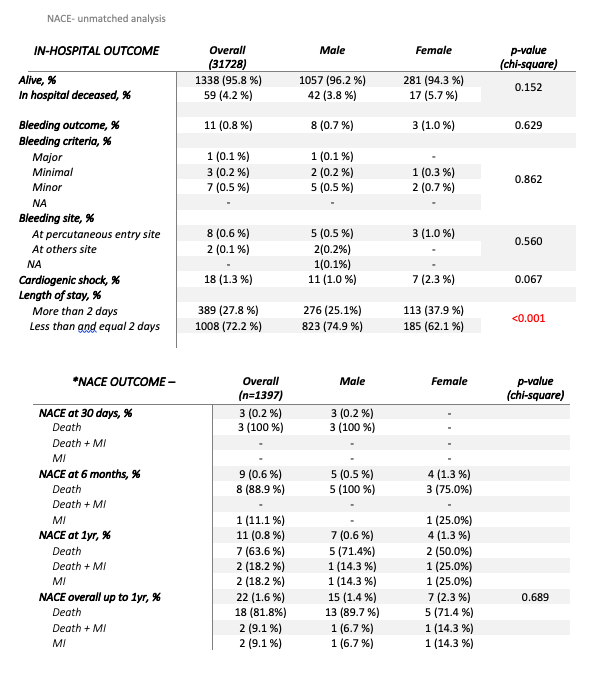
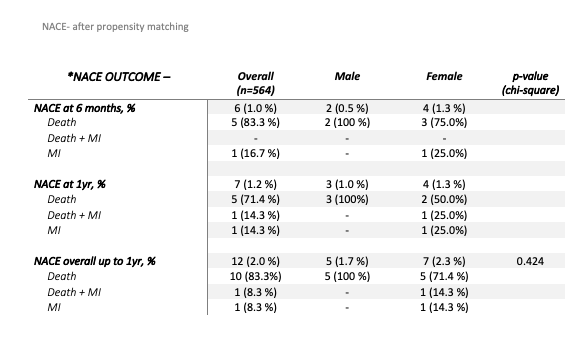
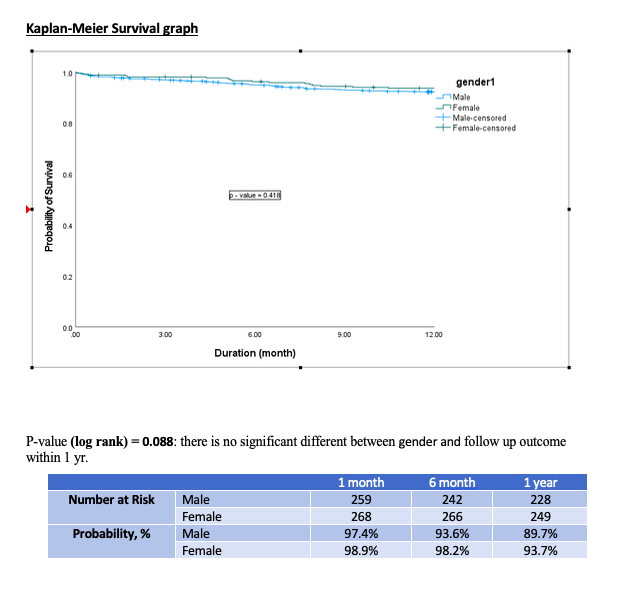
In the unadjusted analysis, compared with men, women had higher risk profiles including age- they were older with 25.5% being more than 70 years old, diabetes mellitus- 63.1%, hypertension- 83.6% and pre-existing heart failure- 8.1% which are all statistically significant. Most of the lesions treated were involving the Distal LMS and were treated with mostly secondary generation DES (87.6% versus 90.3%). The unadjusted rates of NACE were slightly higher for women- Nil versus 0.5% at 30 days, 1.3% versus 0.5% at 6 months, 2.3% vs 1.6% at 1 year. However these differences were not statistically significant (p-value-0.689). There are no significant differences in NACE after propensity matching too (p-value- 0.424). These are further reflected by the Kaplan- Meier survival graph. Logistic regression equation for multivariate analysis reveals that mortality in women is increased 6.4 times in patients with diabetes mellitus and new onset angina. Mortality in men is 3.9 times in patients with renal failure and 2.2 times higher in those with hypertension. Interestingly, females had a longer in hospital stay probably owing to the need of staged procedure in view of the higher incidence of multi-vessel involvement in them.



Conclusion
LMS disease is more common in males and is associated with high mortality rates. Female gender traditionally has been associated with worse overall outcomes post PCI. It is hypothesised that increase risk factors may increase the risk of complications and cardiovascular mortality. However, there is no conclusive evidence whether women have higher mortality and rate of complications in recent times. Hypertension and dyslipidemia are major risk factors of LMS disease in both genders, while smoking is a major risk factor in male patients. Ideally, LMS PCI should be guided by different invasive imagistic methods (IVUS or OCT) or haemodynamic assessment tools (FFR or FFR) which can improve the results of the procedure and the long-term outcomes. From our study, there is a significant increase of mortality rate in women with new onset angina and diabetes mellitus. In patients with diabetes mellitus, coronary angiography would often reveal complex multivessel coronary artery disease involving LMS which challenges the decision making of the best mode of revascularization for the patient. In the DES era, differences between sexes were not observed in relation to long-term Net Adverse Clinical Events (NACE) in patients undergoing unprotected PCI to LMS. Future studies in the form of randomised control trials comparing outcomes among men and women with different modes of revascularization,ie-CABG would be clinically relevant.