HBR patients are also at high ischemic risk and tend to display a significant overlap of HBR with “Complex Higher Risk Indicated Percutaneous Coronary Intervention” or so-called CHIP patients not well-represented in randomized controlled studies.
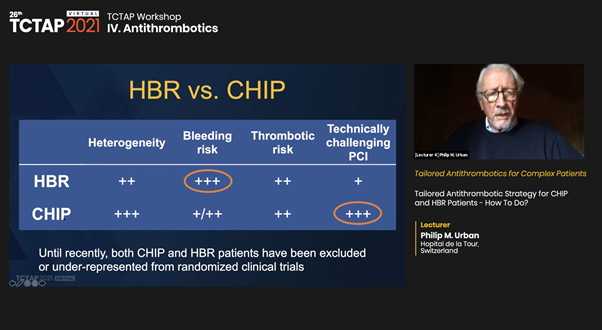
Urban presented on a recently developed and published trade-off model for ARC-HBR patients, designed to predict the risks of major bleeding and myocardial infarction (MI) or stent thrombosis (ST) in HBR patients undergoing PCI.
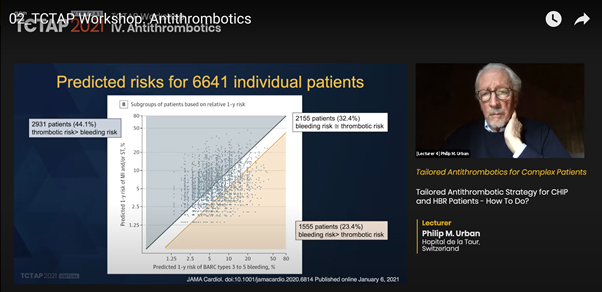
The study, which included more than 12,000 patients, multivariate predictors suggested significant overlap of BARC 3-5 bleeds and ischemic events. About a third of these patients had balanced bleeding vs MI/ST event risk. Furthermore, 44.1 percent were estimated to have higher ischemic risk compared to bleeding risk while 22.4 percent were estimated as higher bleeding risk.
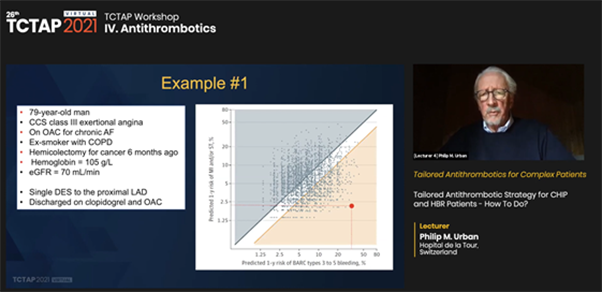
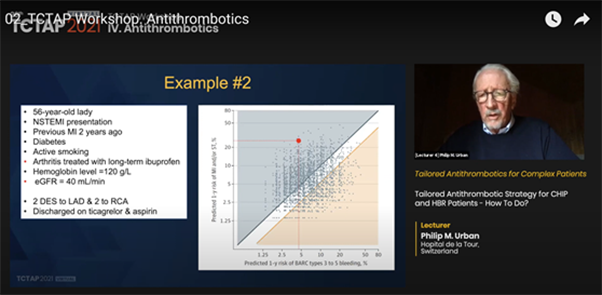
Urban used two case examples that highlighted the use of this predictive model to determine the balance between bleeding and thrombotic risks. While both cases were ARC-HBR, each had a significantly different bleeding-thrombotic risk balance based on the ARC-HBR trade-off model. Urban stressed that the model could enable clinicians to make more measured decisions about their patients.
The ARC-HBR bleeding risk calculator will soon be launched as a phone application to help improve clinician accuracy in gauging the relative balance between bleeding and thrombotic risk in CHIP-HBR patients and better tailor treatment strategies.
Edited by

Jack Wei Chieh Tan, MD
National Heart Centre Singapore, Singapore


