Lots of interesting abstracts and cases were submitted for TCTAP 2021 Virtual. Below are accepted ones after thoroughly reviewed by our official reviewers. Don’t miss the opportunity to explore your knowledge and interact with authors as well as virtual participants by sharing your opinion!
TCTAP A-014
Presenter
Jaryl Ng
Authors
Jaryl Ng1, Valeria Paradies2, Shengjie Lu1, Hwa Liang Leo3, Philip Wong1, Nicolas Foin4, Hui Ying Ang1
Affiliation
National Heart Centre Singapore, Singapore1, Maasstad Hospital, Netherlands2, National University of Singapore, Singapore3, Duke-NUS, Belgium4
View Study Report
TCTAP A-014
Bifurcation/Left Main Diseases and Intervention
Comparison of TAP Stenting and DK Crush Bifurcation Double Stenting Techniques: Insights from an In Vitro Bench Top Study
Jaryl Ng1, Valeria Paradies2, Shengjie Lu1, Hwa Liang Leo3, Philip Wong1, Nicolas Foin4, Hui Ying Ang1
National Heart Centre Singapore, Singapore1, Maasstad Hospital, Netherlands2, National University of Singapore, Singapore3, Duke-NUS, Belgium4
Background
Recently, double stenting techniques had better clinical outcomes compared to single stenting in complex bifurcation lesions. Although there are multiple techniques for double stenting in coronary bifurcation, currently, there is no clear consensus on a superior method to treat bifurcation lesions. In addition, the benefits of final proximal inflation have not been clearly demonstrated. Hence, this study aims to compare two double stenting techniques with regards to restoring the proximal main vessel lumen. Additionally, the impact of final proximal optimization in the proximal main vessel on these techniques were further assessed.
Methods
Left main bifurcation silicon models were deployed with either T-stenting and protrusion (TAP) (n=6) or DK crush(DKC) (n=6) using drug-eluting stents (DES). A final proximal optimization was done after each stent deployment. Optical coherence tomography (OCT) pullbacks were obtained before and after final proximal optimization and were used to measure the cross-sectional area (CSA) and diameters of the stent models. OCT frames in a 5mm segment proximal of the bifurcation ostia were measured for CSA and as well as the maximum and minimum diameters at intervals of 1mm. The eccentricity index (EI) was obtained as a ratio between the maximum and minimum diameter of the measured OCT frame.
Results
Between the two techniques, there was no significant difference observed for CSA (TAP:15.2±2.2mm2, DKC:15.1±1.8mm2,p=0.93) and EI (TAP:1.2±0.1, DKC:1.2 ± 0.1, p=1.0). With regards to the impact of final proximal optimization, TAP showed no significant benefits for both CSA(Before:15.0±0.7mm2, After:15.2±2.2mm2,p=0.84) and EI (Before:1.3±0.2,After:1.2±0.1,p=0.3). For DKC, CSA (Before:14.5±0.8, After:15.1±1.8mm2,p=0.47) showed no significant improvements, but EI (Before:1.4±0.2, After:1.2±0.1,p=0.05) showed significant improvements after final proximal optimization.
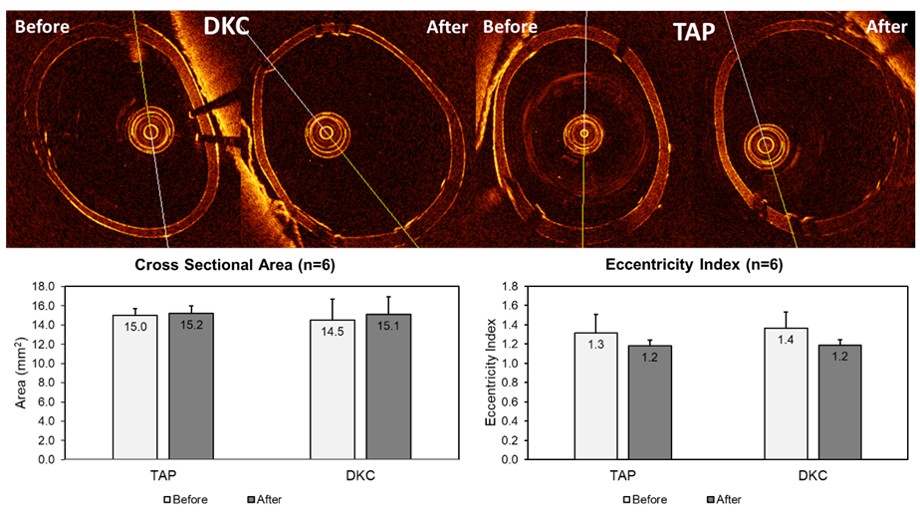

Conclusion
Results show that SB intervention strategies reduce the amount of floating struts in the bifurcation SB ostia, leading to reduced flow disruption and lower acute thrombogenicity compared to KIO method. This bench study is hypothesis-generating as clinical studies have shown no impact of dilating the SB versus not with a single stent provisional stenting strategy.


