Lots of interesting abstracts and cases were submitted for TCTAP 2021 Virtual. Below are accepted ones after thoroughly reviewed by our official reviewers. Don’t miss the opportunity to explore your knowledge and interact with authors as well as virtual participants by sharing your opinion!
TCTAP A-015
Presenter
Bum-Erdene Batbayar
Authors
Khuyag Batmyagmar1, Bum-Erdene Batbayar2, Oyunkhand Buyankhishig1, Surenjav Chimed3, Lkhagvasuren Zundui3
Affiliation
Intermed Hospital, Mongolia1, First State Central Hospital, Mongolia2, Third State Central Hospital, Mongolia3
View Study Report
TCTAP A-015
Bifurcation/Left Main Diseases and Intervention
Impact of Urgent and Elective Percutaneous Coronary Intervention on Outcome of Left Main Coronary Artery Bifurcational Stenosis
Khuyag Batmyagmar1, Bum-Erdene Batbayar2, Oyunkhand Buyankhishig1, Surenjav Chimed3, Lkhagvasuren Zundui3
Intermed Hospital, Mongolia1, First State Central Hospital, Mongolia2, Third State Central Hospital, Mongolia3
Background
Left main coronary artery (LMCA) is large vessel which supplies the majority of left ventricle and critical lesion at the bifurcation of LMCA is possible to induce occlusion of both left anterior descending (LAD) and left circumflex (LCx) arteries and subsequent life-threatening condition. Therefore, percutaneous coronary intervention (PCI) on LMCA bifurcational stenosis is considered as a high-risk procedure. In this study, we aimed to clarify the impact of urgent and elective PCI on outcomes of patients with LMCA bifurcational stenosis.
Methods
We chose patients who received urgent PCI due to acute myocardial infarction (AMI) or elective PCI due to stable coronary artery disease (CAD) for their LMCA bifurcational stenosis. Any lesion with >50% stenosis on coronary angiography was considered as critical stenosis. Bifurcational stenosis was evaluated by Medina classification. All-cause mortality was chosen for the study endpoint. Short (within 30-days) and long term (during follow-up) outcomes were compared by use of Cox proportional hazard regression and Kaplan-Meier method.
Results
A total of 82 patients with LMCA bifurcational stenosis were selected for this study (mean age 62±11, male gender 76.8%) and 14 of them received urgent PCI due to AMI and 68 of them received elective PCI due to stable CAD. Per Medina classification, 27 patients (32.9%) had 111 type lesion,27 patients (32.9%) had 010 type lesion, 12 patients (14.6%) had 110 type lesion, 12 patients (14.6%) had 011 type lesion, 3 patients (3.7%) had 100 type lesion and 1 patient (1.2%) had 101 type lesion. Compared to patients who received elective PCI, patients who received urgent PCI were had significantly higher 30-day mortality (1.5% vs. 21.4%, p<0.05) and all-cause mortality during follow-up (7.4% vs. 35.7%, p<0.003). Urgent PCI for LMCA bifurcation stenosis was significantly associated with higher long term mortality (HR=3.63,95% CI 1.02-12.9, p<0.05) (Figure 1). Kaplan-Meier estimation showed that patients who received urgent PCI have lower survival compared with elective PCI group (Figure 2).
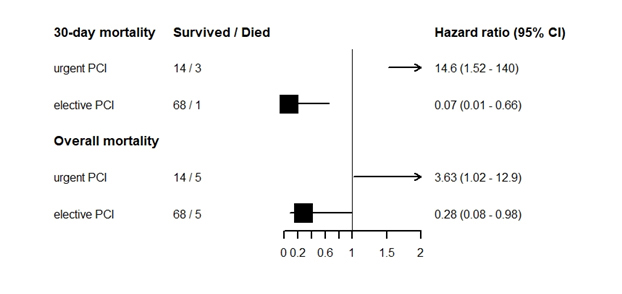
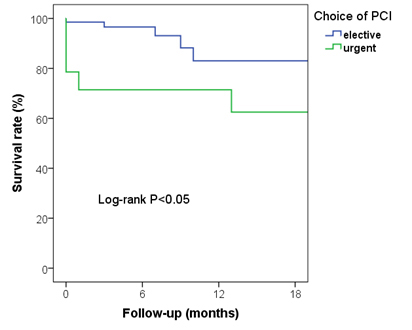


Conclusion
Unanticipated urgent PCI for patients with LMCA bifurcational stenosis due to AMI is associated with higher short and long term mortality and lower survival. Therefore, better screening and planned elective PCI should be considered for patients who suspected LMCA bifurcational stenosis.


